Microfluidics’ potential role in creating accurate wearable technology is significant.
For example, the density of metabolites in sweat — along with its ease of collection from skin pores — make it a useful biofluidic candidate for analysis. One recent study looked at how microchannels and micro reservoirs, pre-filled with fluorescent probes that react to target analytes in sweat, can perform quantitative analysis. To capture sweat, fluorometric sensing modalities were integrated into a skin-interfaced microfluidic system that was paired with a smartphone-based imaging module. This method yielded an accurate measurement of biomarkers in sweat.
In another recent study, researchers developed wearable sensors to monitor biomolecule levels by combining continuous fluid sampling with in-situ analysis. Depending upon the target biomolecule, the particular assay was interchangeable.
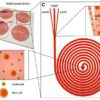
The microfluidic device featured a droplet-flow method for timing, and a micropump to produce nanolitre-sized droplets. Biomarker variations within fluids, over time, yield insight into tissue physiology and may help to create personalized treatments.
The study’s palm-sized sensor autonomously detected deviations from steady-state level.“We demonstrate how the sensor can track perturbed glucose and lactate levels in dermal tissue with results in close agreement with standard off-line analysis and consistent with changes in peripheral blood levels,” the authors wrote.
Biomarker concentrations fluctuate continuously, as does chemical signalling. The capacity for continuous measurement of these dynamics has significant implications.
Many current point-of-care devices are single-measurement tools. The use of microfluidics for continuous monitoring has been strained where microfluidic systems rely upon bulky laboratory equipment such as syringe pumps and microscopes — impractical as wearable devices. But recent advances address this.
For example, the linear nature of microscale flow has required many external control devices. Another recent study, by an international research team, highlights the design of networks with a nonlinear relation between flow rate and its applied pressure. This relation can be harnessed to switch the direction of internal flows by manipulating the input and output pressures.
Using rigid polymer channels to carry water, the investigators showed that these networks demonstrate a fluid version of Braess’s Paradox: closing an intermediate channel resulted in a higher rather than lower, total flow rate. These findings are scalable and can implement flow routing with multiple switches. Practical applications can encompass built-in control mechanisms in microfluidic networks, furthering the creation of portable systems — such as wearable healthcare technologies
These new findings seem to have clear advantages, yet final shepherding of new findings toward commercialization remains the most challenging step. A new device can fail clinically, or it can run out of funding, miscalculate the market, or collide with regulations, according to Georgia Tech benchtop-to-bedside expert Tiffany Wilson.
“Find out about clinical workflow and how health care operates, then maybe decide not to pursue the prototype you had planned, but work on a new one instead,” she warns. “It generally doesn’t work to take what was built in the lab and make the same thing with medical-grade materials, and unfortunately, many researchers don’t realize this until it’s too late.”
And, she notes, “Words matter. For example, if I want to market my new catheter as ‘pain-free,’ the FDA may want me to conduct an expensive clinical trial, but if I take that same catheter and market it as ‘low friction,’ which is why it’s pain-free, then I can demonstrate that with simple bench tests.”
The variety of viewpoints should not be underestimated. “Many stakeholders need their questions answered,” Wilson said. The clinician is only a part of the equation. The hospital supply chain may not be able to handle it. Regulators may not approve it.
“Also, know your competition,” Wilson advised. “Are you more competitive than the current standard of care?”
Yes, we are, microfluidics pioneers can now confirm.
Enjoyed this article? Don’t forget to share.

Kathy Jean Schultz
Kathy Jean Schultz is a freelance medical science writer who focuses on medical innovations. She earned a Master’s Degree in Research Methodology from Hofstra University, and a Master’s Degree in Psychology from Long Island University. She is a member of the National Association of Science Writers, and the Association of Health Care Journalists. Her articles about organoids include "Would you trust a 3-D printed mini organ to test your drugs?" and "Stem cells not only slow disease, they come with their own safety test".