13 Jul Exploring Platelet Generation: Insights from Lung Vasculature and Microfluidic Technology
Platelets play a crucial role in blood clotting and wound healing, but their complex generation process has remained a topic of intense research. In a recent breakthrough, scientists have shed light on the mechanisms of platelet generation using a combination of an ex vivo lung system and cutting-edge microfluidic technology. This innovative approach has not only enhanced our understanding of platelet formation but also holds the potential to revolutionize platelet production for medical applications.
“Using ex vivo lung and an in vitro microfluidic chamber we determine how oxygenation, ventilation, healthy pulmonary endothelium and the microvascular structure support thrombopoiesis. We also show a critical role for the actin regulator Tropomyosin 4 in the final steps of platelet formation in lung vasculature. This work reveals the mechanisms of thrombopoiesis in lung vasculature and informs approaches to large-scale generation of platelets.“, the authors explained.
The lung has emerged as a key site for platelet generation, with reports suggesting it produces a significant portion of total body platelets. By utilizing an ex vivo lung system integrated with a microfluidic device, researchers observed that anuclear fluorescent objects, resembling platelets, were present in the lung vasculature despite undetectable platelets in the perfusate. This finding enabled by microfluidic advancements suggests that the final steps of platelet generation, including enucleation, occur within the lung vasculature. It was also discovered that the protein TPM4 plays a critical role in the transformation of large anuclear fragments into platelets in the lung vasculature.
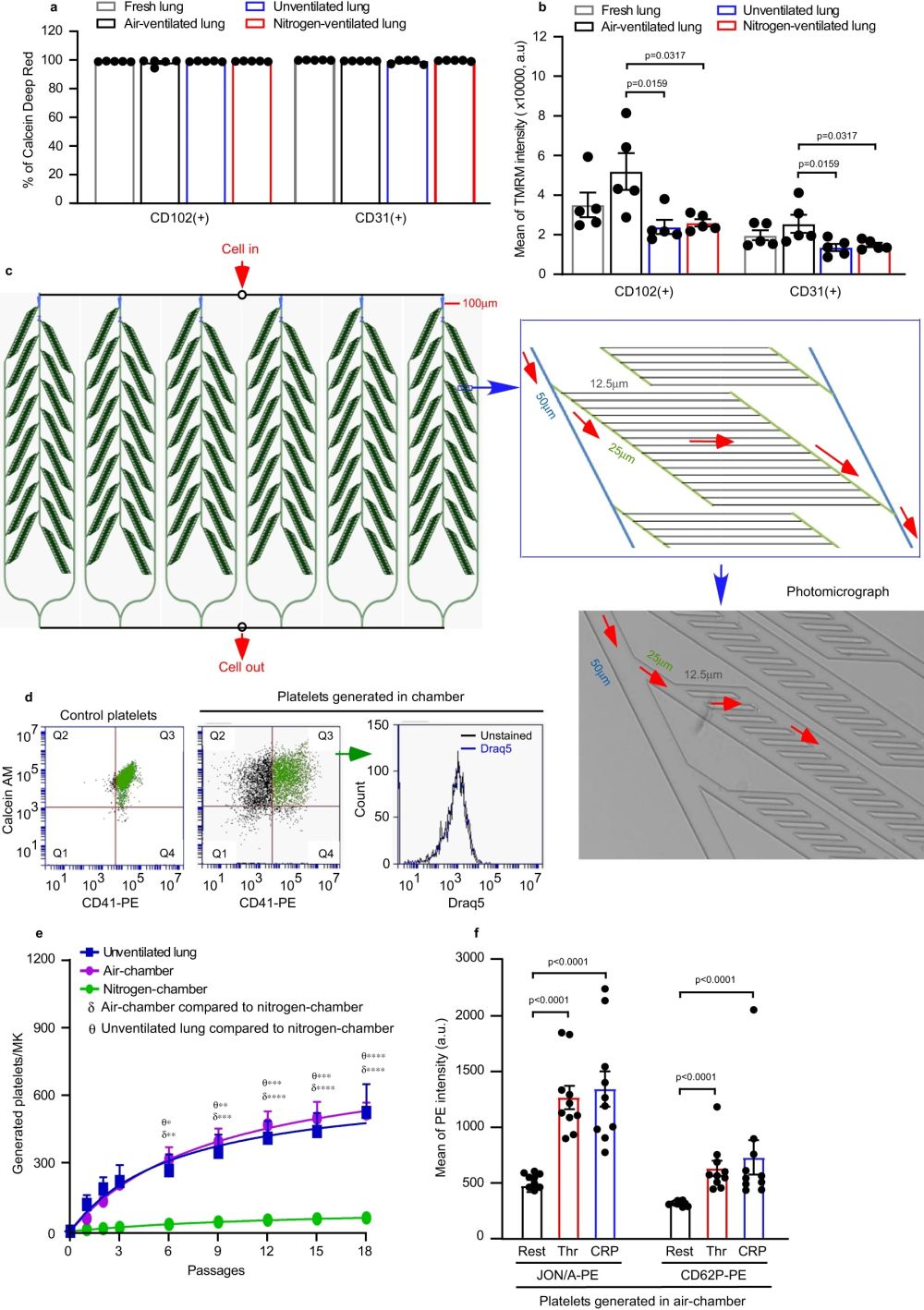
“a, b Pulmonary endothelial cells (ECs) were isolated from perfused lungs under air- (black) or pure nitrogen-ventilation (red) or without ventilation (blue) for ~2 h. ECs from fresh lung tissue served as control (grey). ECs were stained with FITC-conjugated anti-CD31/PECAM-1 or anti-CD102/ICAM-2 antibodies. N = 5 independent experiments for each group. Two-tailed Mann–Whitney test. a Viability of pulmonary ECs were determined by Calcein Deep Red retention and displayed as mean ± SEM. b Mitochondrial membrane potential was determined by accumulation of Tetramethyl rhodamine methyl ester (TMRM) in active mitochondria and displayed as mean fluorescence intensity ± SEM. Air-ventilated lung vs unventilated lung: p = 0.0159 and 0.0159 for CD102 and CD31, respectively. Air-ventilated lung vs nitrogen-ventilated lung: p = 0.0317 and 0.0317 for CD102 and CD31, respectively. c Design of microfluidic chamber simulating a physiological pulmonary vascular system (details shown in Methods), including a photomicrograph of the smallest channels in the system and indication of the flow direction by arrows (red). Dimensions indicated on the figures are width of channels. d, e Mouse megakaryocytes (MKs) prelabelled with CD41-PE were repeatedly pumped through the microfluidic chamber. d The viability of generated platelets from the microfluidic chamber was determined by Calcein AM staining (Generated platelets: CD41+/Calcein AM+ in upper right quadrant, Q3 in green). All generated platelets identified in this way showed no DNA content (DRAQ5 -ve staining). e Quantification of generated platelets per MK in perfusates under air (purple circles) or pure nitrogen conditions (green circles), measured by FACS. For comparison, numbers of platelets generated in the unventilated lung-heart system (blue squares), from Fig. 2a, are shown. N = 4 (for air-chamber or nitrogen-chamber) and 5 (for unventilated lung-heart model) independent experiments. Data are mean ± SEM. Two-way ANOVA with Tukey’s multiple comparisons test, *p < 0.05, **p < 0.01, ***p < 0.001 and ****p < 0.0001. f Mouse MKs prelabelled with CD41-FITC were repeatedly pumped through the microfluidic chamber under air 18 times. Generated platelets were washed and then integrin αIIbβ3 activation and P-selectin expression, induced by 2 U/mL thrombin (Thr) or 5 µg/mL CRP-XL, were measured by FACS. N = 10 independent experiments and data are mean ± SEM. Two-tailed Mann–Whitney test, p < 0.0001. Source data are provided in the Source Data file.” Reproduced from Zhao, X., Alibhai, D., Walsh, T.G. et al. Highly efficient platelet generation in lung vasculature reproduced by microfluidics. Nat Commun 14, 4026 (2023). under Creative Commons Attribution 4.0 International License.
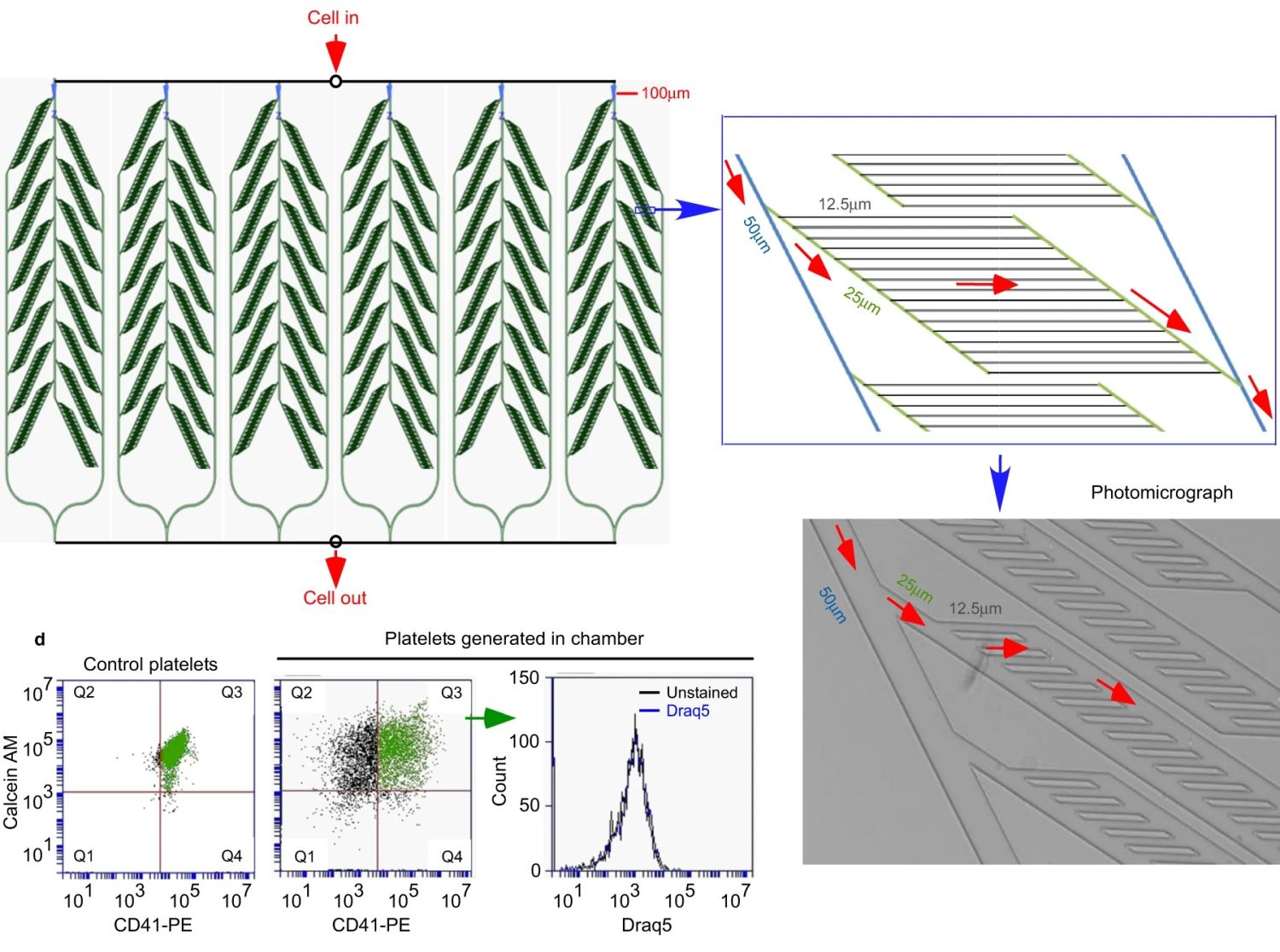
To further investigate platelet generation, researchers developed a microfluidic chip that mimics the capillary channels found in the body. This unique system allowed for the repeated passage of megakaryocytes (MKs) through microchannels, simulating the process within the lung vasculature. By leveraging microfluidic technology, the team achieved efficient platelet generation, with approximately 500 platelets produced per MK. This approach provides a promising avenue for large-scale platelet production outside the body.
The PDMS microfluidic chip used in the study was fabricated through microfluidic fabrication techniques, enabling precise control of channel dimensions and flow parameters. The design involved a branching structure that gradually reduced the channel diameter, resembling the vascular network. By multiplexing in parallel, the researchers scaled up the system to accommodate larger cell volumes, enhancing the efficiency of platelet generation. This demonstrates the power of microfabrication in creating sophisticated devices for biomedical applications.
The findings of this research have far-reaching implications for medicine. Understanding the intricate process of platelet generation opens doors for improved diagnostics and therapies related to platelet disorders and bleeding disorders. Furthermore, the microfluidic system developed in this study provides a promising platform for the large-scale production of platelets for transfusion purposes, potentially addressing the ongoing challenges of platelet shortages.
The combination of an ex vivo lung system and microfluidic technology has unveiled new insights into platelet generation. This research highlights the crucial role of the lung vasculature in platelet formation and showcases the potential of microfluidic devices for large-scale platelet production. As scientists continue to explore this fascinating field, the future of platelet research and medical applications looks promising.
“In summary, this work identifies a highly efficient mechanism for platelet generation outside of the body, by repeated passage of MKs through lung vasculature under air ventilation, involving enucleation and final TPM4-dependent steps to generate platelets. The findings will inform new approaches, such as the microfluidic system reported here, to large scale generation of human platelets. “, the authors explained.
Remember to check our blog for more exciting research highlights and stay up to date with the latest advancements in science and technology!
Figures are reproduced Zhao, X., Alibhai, D., Walsh, T.G. et al. Highly efficient platelet generation in lung vasculature reproduced by microfluidics. Nat Commun 14, 4026 (2023). https://doi.org/10.1038/s41467-023-39598-9
Read the original article: Highly efficient platelet generation in lung vasculature reproduced by microfluidics


